Research Open Access
Doriane Calmes, Pascale Huynen, Virginie Paulus, Monique Henket, Françoise Guissard, Catherine Moermans, Renaud Louis & Florence Schleich
Respiratory Research volume 22, Article number: 76 (2021)
Abstract
Background
Chlamydia pneumoniae and Mycoplasma pneumoniae have been implicated in the pathogenesis of asthma and are responsible for chronic inflammation when host immune system fails to eradicate the bacteria.
Method
We performed a prospective study on 410 patients who underwent a visit at the asthma clinic of CHU of Liege between June 2016 and June 2018 with serology testing for C. pneumoniae and M. pneumoniae.
Results
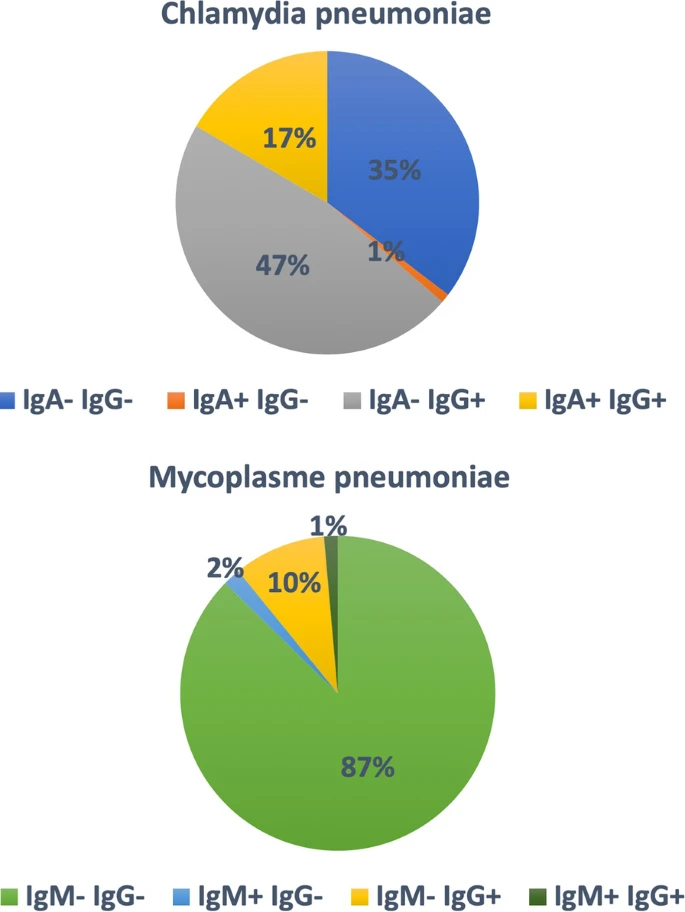
65% of our asthmatic population had serum IgA and/or IgG towards C. pneumoniae, while only 12.6% had IgM and/or IgG against M. pneumoniae. Compared to seronegative asthmatics, asthmatics with IgA+ and IgG+ against C. pneumoniae were more often male and older with a higher proportion of patients with smoking history. They received higher doses of inhaled corticosteroids (ICS) and displayed lower FEV1/FVC ratio, higher RV/TLC ratio and lower conductance. They had higher levels of fibrinogen, though in the normal range and had lower sputum eosinophil counts. Patients with IgA− and IgG+ against C. pneumoniae were older and had higher blood monocyte counts and alpha-1-antitrypsin levels as compared to seronegative patients. Patients with IgM and/or IgG towards M. pneumoniae were more often males than seronegative asthmatics. In a subpopulation of 14 neutrophilic asthmatics with Chlamydia pneumoniae IgA + /IgG + treated with macrolides, we found a significant decrease in blood neutrophils and normalization of sputum neutrophil count but no effect on asthma quality of life and exacerbations.
Conclusion
Positive Chlamydia serologic test is more common than positive Mycoplasma serology. Asthmatics with IgA and IgG against C. pneumoniae have more severe disease with increased airway obstruction, higher doses of ICS, more signs of air trapping and less type-2 inflammation.
