Research – Open Access
Patrizia Pignatti, Dina Visca, Francesca Cherubino, Elisabetta Zampogna, Etienne Lucini, Laura Saderi, Giovanni Sotgiu and Antonio Spanevello
Introduction
Airway eosinophilic inflammation is a characteristic of asthmatic patients and of a sub group of COPD subjects. Blood eosinophils are deemed as a good surrogate marker of sputum eosinophilic inflammation; however, controversial data have been published particularly in COPD. The aim of our study was to compare blood and sputum eosinophils in COPD and asthmatic patients in “real life”.
Methods
Sputum was induced in stable patients with COPD or asthma with hypertonic saline solution and blood eosinophils were evaluated. Frequency of comorbidities was recorded. Correlations were performed stratifying patients by disease and comorbidities.
Results
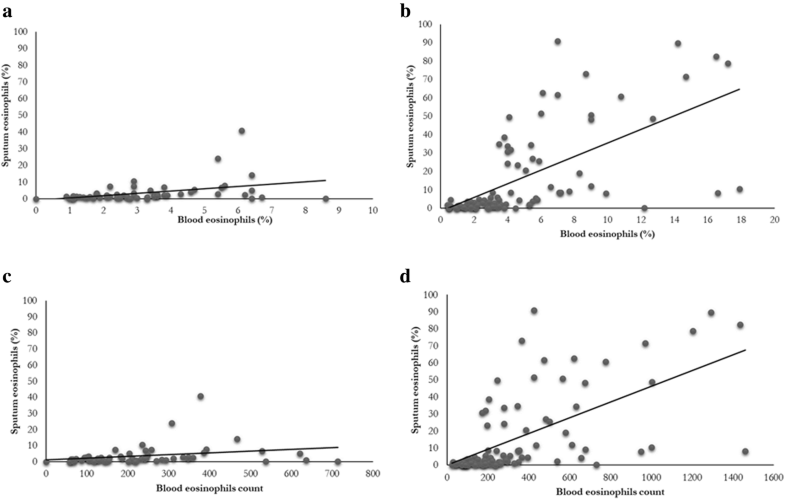
146 patients, 57 with COPD and 89 with asthma were evaluated. Blood and sputum eosinophils expressed as percentages were correlated in COPD (rho = 0.40; p = 0.004), but the entity of correlation was lower compared with asthmatic subjects (rho = 0.71; p < 0.0001). When blood eosinophils were expressed as counts the correlation was slightly lower than when expressed as percentages in COPD (rho = 0.35; p = 0.01) and in asthmatic patients (rho = 0.68; p < 0.0001). In COPD patients older than 73 years or with blood eosinophils higher than the median value (210.6 eos/μl), or co-diagnosed with hypertension, ischemic heart disease or atrial fibrillation no correlation between blood and sputum eosinophils was found.
However, the effect of ischemic heart disease and atrial fibrillation could be driven by hypertension since most of these patients have this comorbidity.
Conclusion
Blood eosinophils correlated with sputum eosinophils to a lesser degree in COPD than in asthmatic patients. Older age, high blood eosinophils and hypertension affected the correlation between blood and sputum eosinophils, more studies are needed to evaluate the role of other cardiac comobidities.
