Research – Open Access
Kristi J. Warren, Jill A. Poole, Jenea M. Sweeter, Jane M. DeVasure, John D. Dickinson, R. Stokes Peebles Jr & Todd A. Wyatt
Respiratory Research volume 22, Article number: 206 (2021)
Abstract
Background
Respiratory viral infections are one of the leading causes of need for emergency care and hospitalizations in asthmatic individuals, and airway-secreted cytokines are released within hours of viral infection to initiate these exacerbations. IL-33, specifically, contributes to these allergic exacerbations by amplifying type 2 inflammation. We hypothesized that blocking IL-33 in RSV-induced exacerbation would significantly reduce allergic inflammation.
Methods
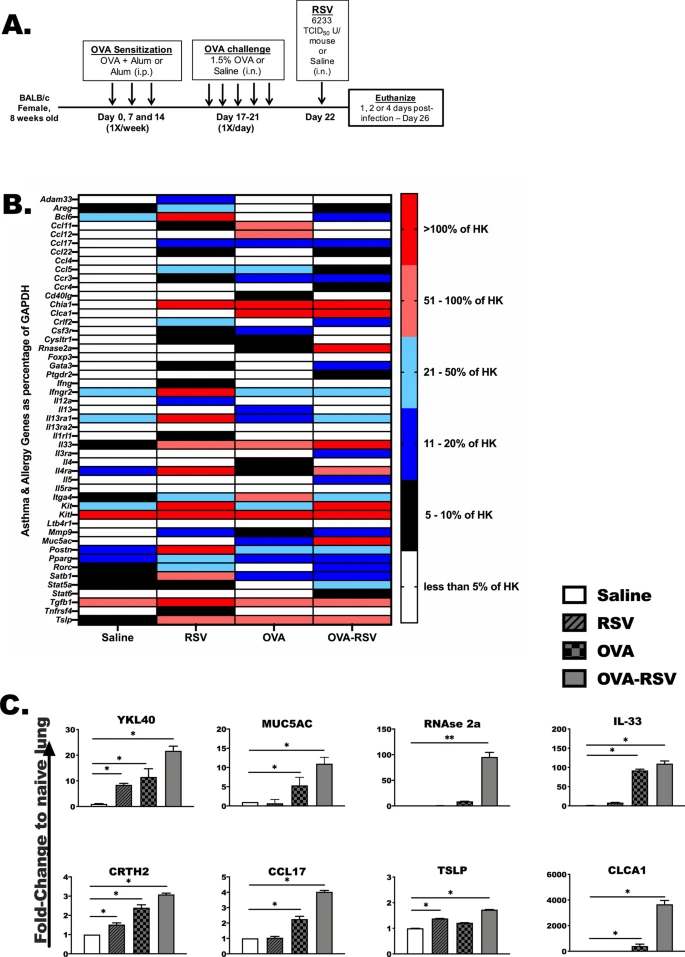
Sensitized BALB/c mice were challenged with aerosolized ovalbumin (OVA) to establish allergic inflammation, followed by RSV-A2 infection to yield four treatment groups: saline only (Saline), RSV-infected alone (RSV), OVA alone (OVA), and OVA-treated with RSV infection (OVA-RSV). Lung outcomes included lung mRNA and protein markers of allergic inflammation, histology for mucus cell metaplasia and lung immune cell influx by cytospin and flow cytometry.
Results
While thymic stromal lymphopoietin (TSLP) and IL-33 were detected 6 h after RSV infection in the OVA-RSV mice, IL-23 protein was uniquely upregulated in RSV-infected mice alone. OVA-RSV animals varied from RSV- or OVA-treated mice as they had increased lung eosinophils, neutrophils, group 2 innate lymphoid cells (ILC2) and group 3 innate lymphoid cells (ILC3) detectable as early as 6 h after RSV infection. Neutralized IL-33 significantly reduced ILC2 and eosinophils, and the prototypical allergic proteins, IL-5, IL-13, CCL17 and CCL22 in OVA-RSV mice. Numbers of neutrophils and ILC3 were also reduced with anti-IL-33 treatment in both RSV and OVA-RSV treated animals as well.
Conclusions
Taken together, our findings indicate a broad reduction in allergic-proinflammatory events mediated by IL-33 neutralization in RSV-induced asthma exacerbation.
