Research, Open Access
Dirk Koschel, Claudia Mailänder, Inessa Schwab Sauerbeck & Jens Schreiber
Allergy, Asthma & Clinical Immunology volume 16, Article number: 92 (2020)
Abstract
Background
This differential diagnosis of allergic vs non-allergic asthma is typically made on the basis of sensitization to allergens, such that absence of sensitization could result in a patient being managed as having non-allergic asthma. In Germany, the number of specific allergen tests is limited and non-standardized (across clinicians and laboratories), with the potential for false negative diagnoses. IDENTIFY aimed to gain data on sensitizations toward aeroallergens in patients with severe asthma who had tested negative to perennial aeroallergens in previous tests.
Methods
This was a single visit, non-randomized, non-interventional study conducted in 87 centers across Germany. The only inclusion criteria were that patients had to be adults (at least 18 years of age) with a diagnosis of severe asthma (receiving at least Global Initiative for Asthma Step IV therapy), and who had previously tested negative to perennial aeroallergens. Patients were then tested for sensitization to a panel of 35 perennial aeroallergens, with positive sensitization indicated by CAP ≥ 0.35 kU/L.
Results
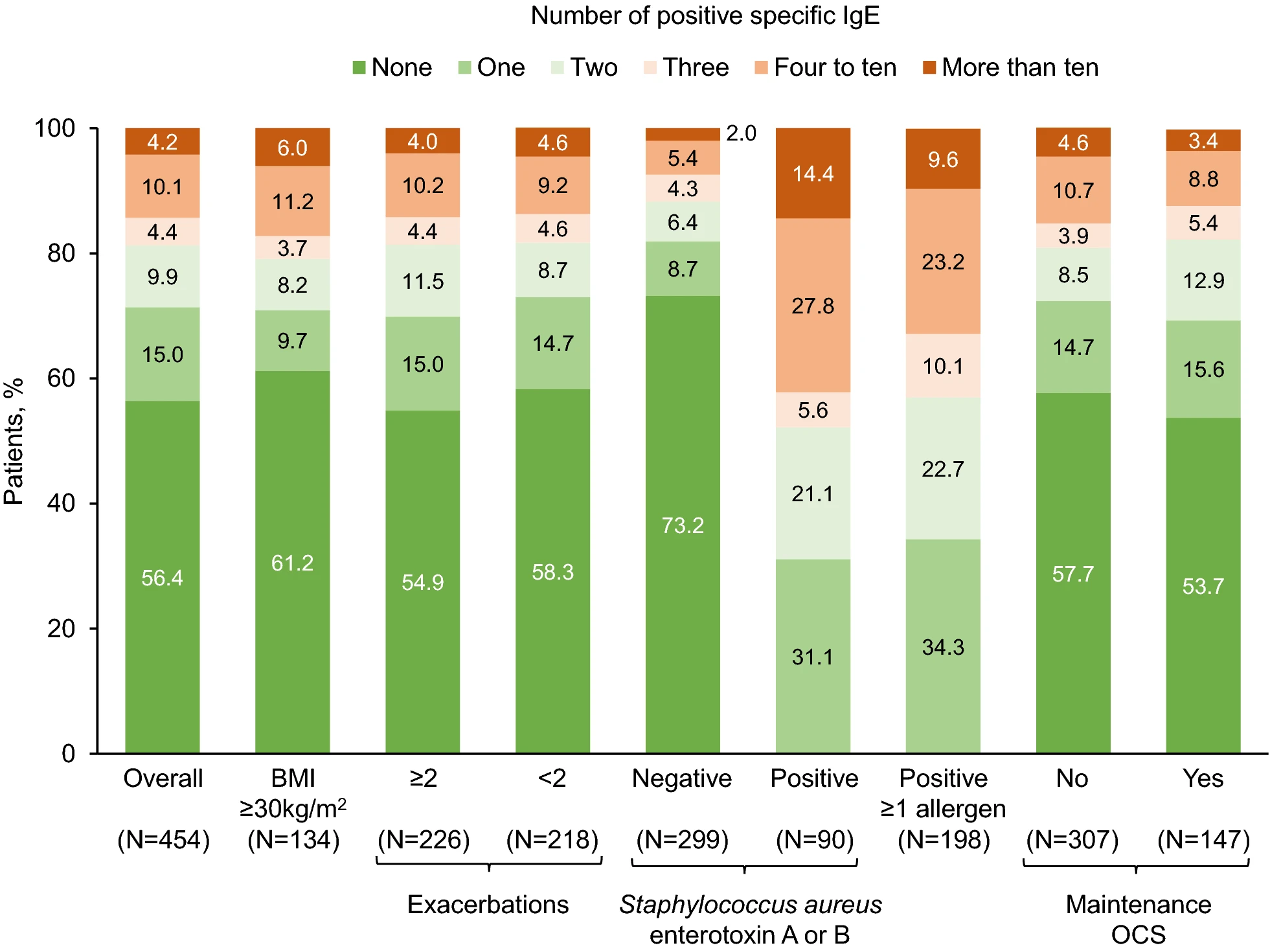
Of 588 patients recruited, 454 had complete and valid data, and had previously tested negative to perennial aeroallergens. Overall, 43.6% of the analyzed patients tested positive for at least one of the included aeroallergens, with 18.7% testing positive for three or more, and 4.2% positive for more than ten. The five most common sensitizations were to Staphylococcus aureus enterotoxin B, Aspergillus fumigatus, Candida albicans, Dermatophagoides farinae, and Rhizopus nigricans, each of which tested positive in at least 9.7% of the population.
Conclusions
In this group of patients being managed as having non-allergic asthma (and who had all previously tested negative to perennial aeroallergens), a high proportion tested positive to a broad panel of aeroallergens. A diagnosis of allergic asthma therefore cannot be excluded purely on the basis of standard aeroallergen panels.
