
Caminati, M., Vatrella, A., Rogliani, P. et al. Respir Res 25, 367 (2024). https://doi.org/10.1186/s12931-024-02998-6
Abstract
Background
An increasing amount of evidence supports the relevance of epithelium across the wide spectrum of asthma pathobiology. On a clinical ground tezepelumab, selectively binding TSLP, a major epithelial cytokine, has demonstrated to be effective in asthma patients regardless their specific phenotype. In order to avoid the risk of considering tezepelumab as a not-specific option, the present perspective aims to sketch the tezepelumab best eligible patient profile and to propose some hallmarks of epithelial-driven disease by reviewing the published evidence on the drug mechanism of action and efficacy data.
Main body
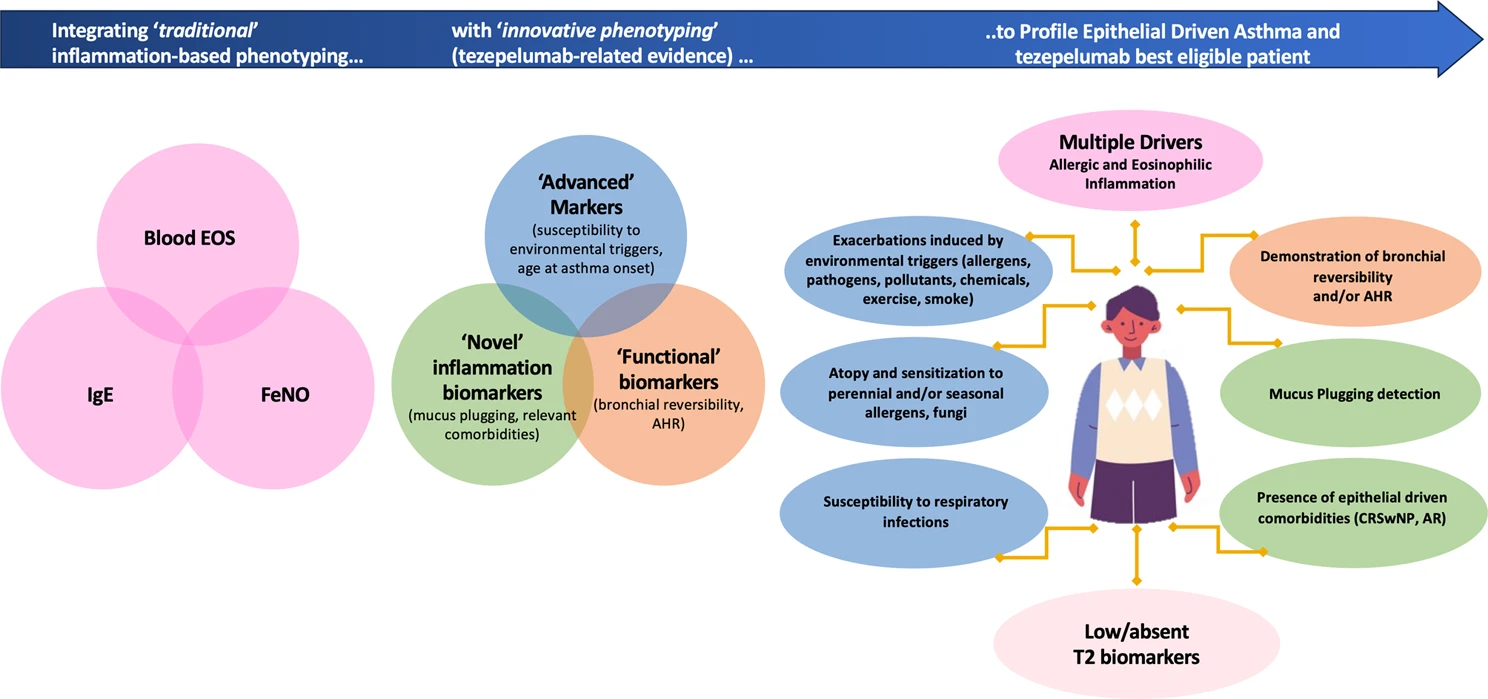
Although it cannot rely on standardised or exclusive “markers”, the relationship between environment and poor asthma control might suggest a major relevance of the epithelial barrier dysfunction. In that light, allergy and asthma exacerbations concomitant with specific exposures (pathogens, pollutants, chemicals), as well as increased susceptibility to infections can be considered as the hallmark of an impaired epithelial immune response. Tezepelumab is effective in allergic patients, being able to reduce asthma exacerbations precipitated by the exposure to seasonal or perennial aeroallergens, including fungi. In addition, tezepelumab reduced the incidence of co-occurring respiratory illness and asthma exacerbations. In terms of inflammation, epithelial immune response has been related to an impaired mucus hypersecretion and plugging. A placebo-controlled trial demonstrated a significant reduction of mucus plugging in treated patient. Airways hyperreactivity (AHR), airways obstruction and remodelling have been described as an expression of epithelial orchestrated immunological activation. Of note, a significantly higher incidence of mannitol negative test in patients treated with tezepelumab when compared to placebo group has been observed. In addition, A 130 mL improvement in pre-BD FEV1 has been described in patients assuming Tezepelumab. The above-mentioned data suggest that bronchial reversibility and AHR can be considered “functional biomarkers” supporting patients’ phenotyping and the identification of tezepelumab best responders.
Conclusion
Integrating “functional biomarkers” to the inflammatory ones and a better characterization of asthma exacerbations might pave the way to a different and more transversal phenotyping, which overcomes the “restrictive” labels including T2 high, allergic/atopic or T2 low asthma. Precisely defining the disease characteristics and potential targets for a better control even in tezepelumab eligible subjects is essential to avoid the block buster temptation and optimize the personalized medicine approach according to each patient’s individuality.
