Research – Open Access
Jian Luo, Yi-Ling Chen, Wentao Chen, David A. Duncan, Alexander Mentzer, Julian C. Knight, Graham Ogg, Paul Klenerman, Ian D. Pavord & Luzheng Xue
Allergy, Asthma & Clinical Immunology volume 17, Article number: 67 (2021)
Abstract
Background
A significant portion of COVID-19 sufferers have asthma. The impacts of asthma on COVID-19 progression are still unclear but a modifying effect is plausible as respiratory viruses are acknowledged to be an important trigger for asthma exacerbations and a different, potentially type-2 biased, immune response might occur. In this study, we compared the blood circulating cytokine response to COVID-19 infection in patients with and without asthma.
Methods
Plasma samples and clinical information were collected from 80 patients with mild (25), severe (36) or critical (19) COVID-19 and 29 healthy subjects at the John Radcliffe Hospital, Oxford, UK. The concentrations of 51 circulating proteins in the plasma samples were measured with Luminex and compared between groups.
Results
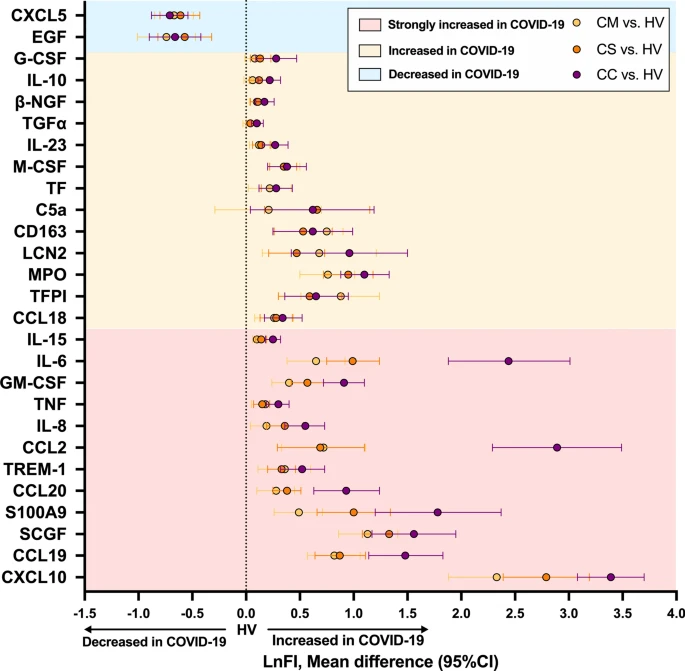
Total 16 pre-existing asthma patients were found (3 in mild, 10 in severe, and 3 in critical COVID-19). The prevalence of asthma in COVID-19 severity groups did not suggest a clear correlation between asthma and COVID-19 severity. Within the same COVID-19 severity group, no differences were observed between patients with or without asthma on oxygen saturation, CRP, neutrophil counts, and length of hospital stay. The mortality in the COVID-19 patients with asthma (12.5%) was not higher than that in patients without asthma (17.2%). No significant difference was found between asthmatic and non-asthmatic in circulating cytokine response in different COVID-19 severity groups, including the cytokines strongly implicated in COVID-19 such as CXCL10, IL-6, CCL2, and IL-8.
Conclusions
Pre-existing asthma was not associated with an enhanced cytokine response after COVID-19 infection, disease severity or mortality.
